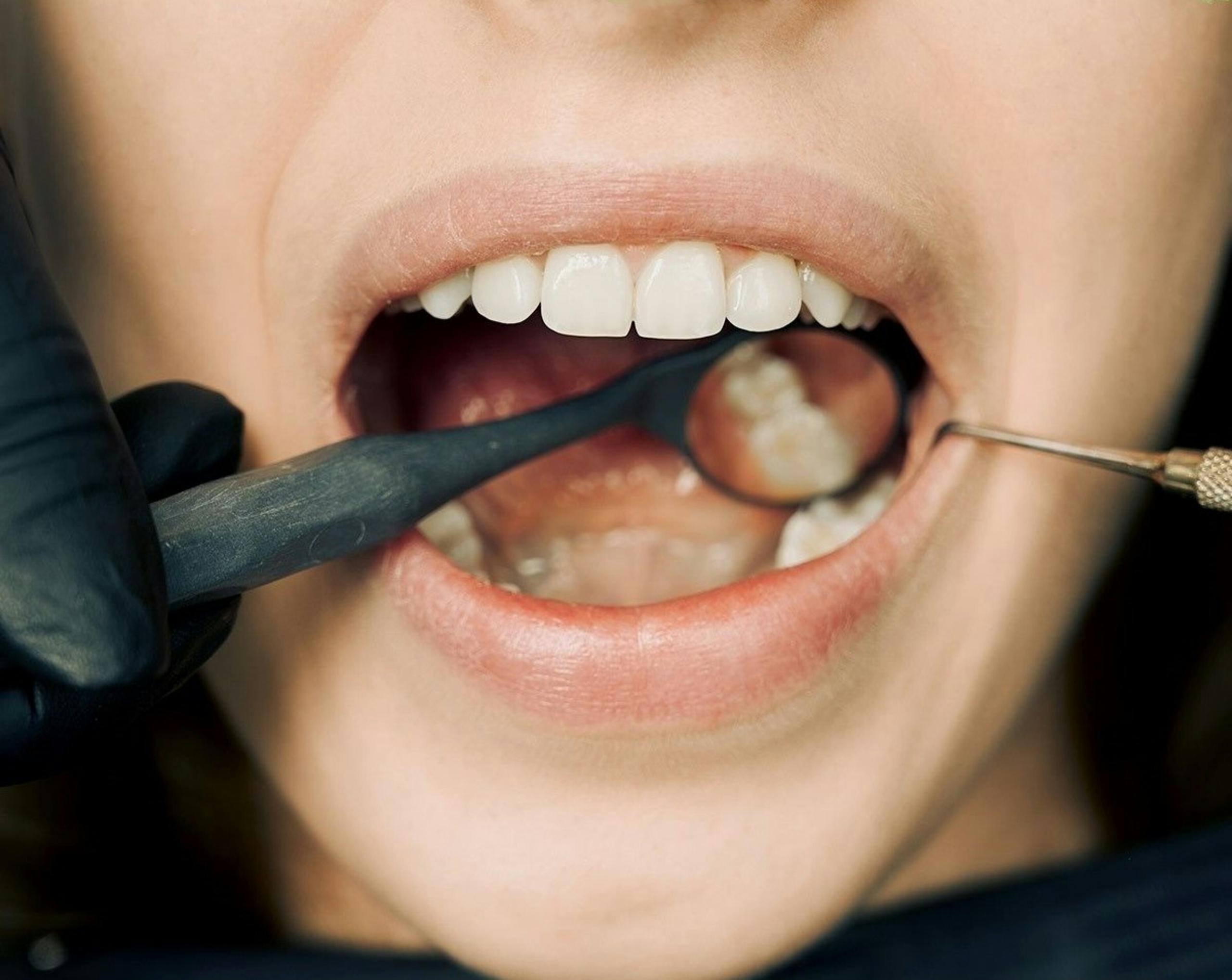
Why Dentists Ask About Diabetes When Gums Bleed
Why your dentist asks about diabetes when your gums bleed
Bleeding gums do not automatically mean diabetes. Gum bleeding is common with gingivitis, plaque buildup, and missed cleaning between teeth. But diabetes can make gum inflammation more likely, and it can also affect dry mouth and how quickly your mouth heals.
That is why a dentist may ask about diabetes when gums look swollen, bleed easily, or seem slow to settle down. The question is usually about safer planning, not judgment.
The gum disease and diabetes connection in plain language
The relationship goes both ways. Diabetes can make it harder for gums to stay healthy, especially when blood sugar is not well controlled. At the same time, ongoing gum disease can add inflammation in the mouth, and treating periodontitis may modestly improve blood sugar control in people who already have both diabetes and periodontitis.
That said, dental care does not replace medical diabetes care. It is one part of the overall picture.
Also, diabetes is not the only reason gums bleed. Brushing and flossing habits, plaque and tartar buildup, dry mouth, smoking, certain medicines, and other oral conditions can all play a role. That is why the cause should be looked at case by case.
What to tell the dental team before or during the visit
If you are coming in with bleeding or swollen gums, it helps to share a few details:
- whether you have diabetes, prediabetes, or are being checked for it
- any recent A1C or glucose information you already know
- a current medication list, including insulin or other diabetes medicines
- any dry mouth, frequent thirst, or mouth soreness
- whether cuts, sores, or dental work have healed slowly before
- any new changes in gum bleeding, swelling, or bad taste
You do not need perfect numbers. Even a simple history can help the dental team choose the right pace and level of follow-up.
What the dentist may look for and why coordination matters
During the exam, the dentist may look for signs of inflammation, deeper gum pockets, plaque and tartar, bleeding points, gum recession, and dryness in the mouth. They may also ask about your home care routine and any recent changes in healing.
If the gums look more inflamed than expected, or if healing seems slower than it should, the dentist may talk with you about next steps. That might include a cleaner, closer follow-up, or a note to check in with the clinician who helps manage your diabetes. Care should be individualized, because diabetes control, dry mouth, smoking, other health conditions, and the state of the gums all matter.
What you can do at home to support gum health
Good home care still matters a lot. The basics are simple, but they work best when done consistently:
- brush twice a day with fluoride toothpaste
- clean between your teeth once a day
- keep regular dental follow-up visits
- ask your dental team what is realistic for your situation if your mouth is sore, dry, or hard to clean
If you already have diabetes, gum care is not an extra detail to ignore. It is part of protecting the tissues that hold your teeth in place.
A calm next step for Hamilton patients and families
If you are in Hamilton and you have questions about bleeding gums, diabetes, dry mouth, or slow healing, bring them to a regular checkup. At Excel Dental, the goal is to review what is happening, explain it in plain language, and help you decide what follow-up makes sense based on your health history.
Sources
- Diabetes Canada: Diabetes and Your Teeth
- Government of Canada Oral Health for Adults
- Cochrane Review: Treatment of Periodontitis for Glycaemic Control in People with Diabetes Mellitus
- EFP Recommendations on Periodontitis and Diabetes for Medical Settings
- Framework for Diabetes in Canada
- Canada
- Publichealthontario
- Perio
- Pubmed
- Pubmed
- Pubmed
This article is for general education only and does not replace personalized advice, diagnosis, or treatment from a licensed dentist.