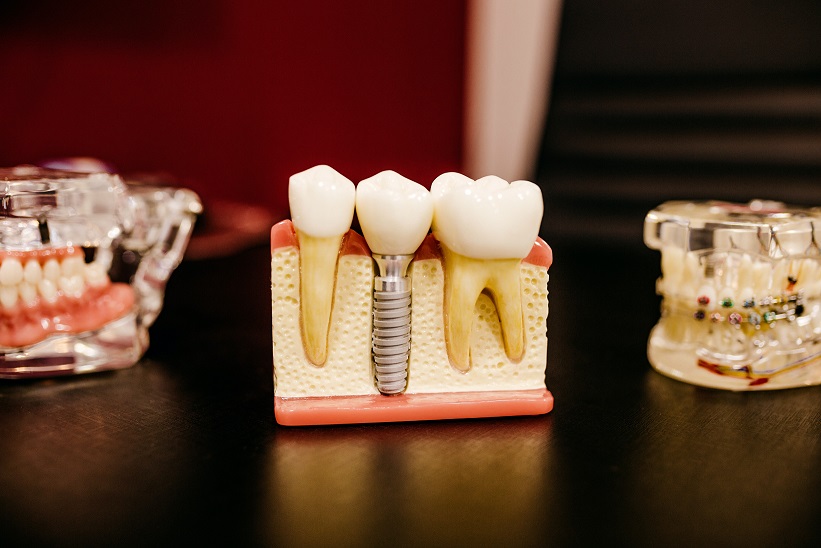
Dental Implants and Bone Support: How to Protect the Bone Around an Implant Before and After Treatment
What bone support means around a dental implant
A dental implant does not just depend on the metal post itself. It also depends on the bone and gum tissue around it. That supporting bone helps keep the implant stable, comfortable, and able to handle everyday chewing over time.
When the bone around an implant stays healthy, the implant is more likely to function well. When that bone is gradually lost, the implant may become harder to clean, less comfortable, or less stable. In more advanced cases, treatment can become more complex.
This is why bone support matters before treatment, during healing, and long after the final crown or bridge is placed. Implant care is not only about the day of surgery. It is also about planning, daily home care, and ongoing professional maintenance.
Why bone can be lost around an implant
Bone loss around an implant can happen for different reasons. A major concern is peri-implant disease, which affects the tissues around implants. The American Academy of Periodontology explains that peri-implant mucositis involves inflammation in the soft tissue around an implant without bone loss, while peri-implantitis includes inflammation plus loss of the supporting bone.
Patients cannot confirm this at home on their own. Bleeding, tenderness, or soreness can be warning signs, but they do not automatically mean peri-implantitis. Diagnosis depends on a clinical exam, comparison over time, and imaging when appropriate.
The European Federation of Periodontology peri-implant disease guideline emphasizes prevention, early detection, and recurrence prevention. In practical terms, that means keeping plaque under control, checking implants regularly, and monitoring changes instead of waiting until symptoms become obvious.
Risk factors your dentist will review before treatment
Not every patient has the same risk of bone loss around an implant. Before treatment, your dentist should review factors that can affect healing, stability, and long-term maintenance.
Common risk factors include:
- Plaque buildup and difficulty cleaning around the implant site
- A history of gum disease
- Smoking or nicotine use
- Poorly controlled diabetes
- Excess biting forces or clenching and grinding
- Bone volume and gum tissue conditions at the planned implant site
- Implant and restoration design factors that may affect cleanability and force distribution
The 2025 AAP and Academy of Osseointegration peri-implant consensus reinforces that risk factors matter both before and after treatment. Some risks can be modified, while others need closer monitoring and a more personalized maintenance plan.
In Ontario, the RCDSO implant dentistry guideline also supports a careful planning process. That includes a full medical and dental history, a clinical examination, and appropriate radiographs for the site being considered. For some patients, additional imaging may be needed. The goal is not to order tests routinely without reason, but to gather enough information to plan safely and realistically.
What helps protect bone before treatment
Protecting bone starts before the implant is placed. Good planning helps reduce avoidable problems later.
Before treatment, your dentist may discuss:
- Whether the bone and gum support at the site are adequate
- Whether past gum disease needs to be stabilized first
- Whether smoking cessation or better diabetes control would improve the outlook
- How the future crown, bridge, or denture will be shaped so you can clean around it well
- Whether clenching or grinding should be addressed
- What the alternatives are if an implant is not the best option right now
Consent also matters. The RCDSO consent to treatment standard supports discussing benefits, material risks, expected limitations, and reasonable alternatives. For implants, that conversation should also include the ongoing maintenance commitment. An implant is not a one-time product. It is a treatment that needs long-term care.
Daily habits and professional care that help protect bone
Once an implant is in place, daily plaque control becomes part of protecting the bone around it. Even a well-placed implant can run into trouble if the surrounding tissues are not kept clean.
Helpful daily habits often include:
- Brushing carefully along the gumline around the implant
- Cleaning between the implant and nearby teeth with floss, interdental brushes, or other tools recommended for your specific restoration
- Following the home-care plan your dental team shows you, rather than guessing
- Avoiding tobacco when possible
- Keeping medical conditions, including diabetes, as well controlled as you can with your physician and dental team
The European Federation of Periodontology prevention recommendations infographic highlights practical prevention steps such as baseline measurements, repeat checks over time, individualized oral hygiene instruction, and supportive care that matches the patient’s level of risk.
That last point is important. There is no single recall interval that fits everyone. Some people do well with less frequent maintenance, while others need closer follow-up because of gum disease history, smoking, dexterity challenges, or more complex restorations. Supportive peri-implant care should be tailored to the patient, not assigned as a one-size-fits-all schedule.
Professional checks matter because some bone changes are subtle at first. Your dentist may compare gum measurements, check for bleeding or inflammation, review how the restoration fits and functions, and take imaging when the exam suggests it is needed. As the RCDSO implant dentistry guideline notes, radiographic assessment may help, but it does not replace an appropriate clinical evaluation.
Warning signs patients may notice at home
You may not be able to diagnose bone loss at home, but you may notice changes that deserve an appointment.
Book a dental visit if you notice:
- Bleeding when brushing or cleaning around an implant
- Swollen, red, or tender gum around the implant
- A persistent bad taste or bad smell from the area
- Pus or discharge
- A restoration that suddenly feels different, loose, or mobile
- New discomfort when biting or a bite that feels off
These signs do not prove bone loss, and they do not always mean the implant itself is failing. Sometimes the problem is limited to the soft tissue. Sometimes the issue is with the crown, screw, bite forces, or trapped plaque. But they are good reasons to have the area checked sooner rather than later.
Why regular supportive care is part of implant treatment
Many patients think of implant treatment as surgery plus a final tooth. In reality, maintenance is part of the treatment from the beginning.
Regular supportive care gives your dental team a chance to compare what they see today with your baseline records, monitor for early changes, and intervene before more bone is affected. Early changes around an implant may be easier to manage than advanced disease.
This is one reason implant follow-up should not be treated as an optional extra. It is part of protecting your investment in comfort, function, and daily quality of life.
Questions to ask your dentist about implant maintenance and bone monitoring
If you already have an implant, or you are planning one, these questions can help you understand the long-term plan:
- How will my bone and gum support be checked before treatment?
- What risk factors in my history could affect bone loss around an implant?
- How will you make sure the final restoration is easy enough for me to clean?
- What baseline measurements will you record after the implant is restored?
- How often should my implant be reviewed based on my own risk level?
- What warning signs should lead me to book sooner?
- If I have a history of gum disease, how does that change my maintenance plan?
- Would a night guard or bite adjustment help protect the implant if I clench or grind?
Practical takeaway
Dental implants can do very well, but the supporting bone still needs lifelong care. The best protection usually comes from good planning, realistic consent, daily cleaning, and supportive follow-up that fits your risk level.
If you are considering an implant, ask not only how the tooth will be replaced, but also how the bone and gums around it will be measured and monitored over time. If you already have an implant and notice bleeding, swelling, tenderness, a bad taste, or a change in comfort, it is worth booking an exam. Small problems are often easier to manage before more supporting bone is affected.
Sources
- EFP Guideline on Peri-Implant Diseases
- EFP Prevention Recommendations Infographic
- AAP and AO Consensus on Peri-Implant Diseases
- AAP Peri-Implant Diseases
- RCDSO implant dentistry guideline
- RCDSO consent to treatment standard
- RCDSO Standards and Guidance
- Government of Canada Oral Health
- Efp
- Pubmed
- Pubmed
- Rcdso
- Rcdso
This article is for general education only and does not replace personalized advice, diagnosis, or treatment from a licensed dentist.